Highlights
- Pulsed and continuous photobiomodulation (PBM) may produce distinct biological effects.
- Pulsed light can reduce tissue heating while allowing higher peak power delivery.
- Evidence suggests pulsed PBM may enhance penetration and biological responses in some conditions.
- Multiple mechanisms have been proposed, including ion channel modulation and nitric oxide dynamics.
- Clinical evidence is heterogeneous, with both pulsed and continuous modes showing therapeutic benefits.
Background and Rationale
Photobiomodulation (PBM), also known as low-level laser therapy (LLLT), has been widely used for tissue repair, pain modulation, and inflammation control. However, a key unresolved question remains: should PBM be delivered in continuous wave (CW) or pulsed wave (PW) mode? This distinction may influence biological responses at cellular and systemic levels, and has been explored in the scientific literature over several decades.
Key Mechanisms and Biophysical Differences
Thermal and Energy Dynamics
Pulsed PBM introduces “off” periods between emissions, allowing:
- Reduced tissue heating
- Higher peak power delivery
- Improved safety in deeper tissues
Continuous wave (CW), in contrast, delivers constant energy and may increase thermal load depending on parameters.
Depth of Penetration
Wavelength remains the primary determinant of penetration; however, pulsed light may improve effective depth due to higher peak power. Still, real clinical differences are likely modest and depend on dosimetry.
Cellular and Molecular Interactions
Proposed mechanisms include:
- Ion channel kinetics (millisecond-scale biological processes)
- Possible resonance with brain wave frequencies
- Repeated nitric oxide (NO) photodissociation enhancing mitochondrial signaling
These mechanisms remain under investigation but are supported by experimental observations.
Evidence from Preclinical and Clinical Studies
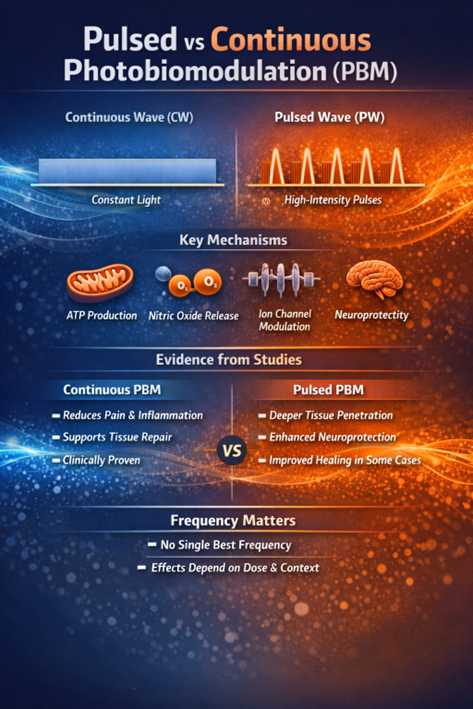
Pulsed vs Continuous
- Pulsed and continuous PBM are both effective, with many studies suggesting advantages for pulsed delivery, although results are not consistent.
- Both modes reduce pain, with pulsed PBM potentially producing stronger or longer-lasting effects.
- PBM supports tissue repair, with some evidence favoring pulsed light in wound healing.
- In neurological models, pulsed PBM has shown enhanced neuroprotective effects and increased ATP production.
- No single optimal pulse frequency exists; biological responses are nonlinear and depend on context and parameters.
Takeaway
Pulsed and continuous PBM are complementary approaches rather than competing ones. The optimal choice depends on the clinical goal, tissue target, and parameter selection.
Reference: Hashmi, J. T., Huang, Y. Y., Sharma, S. K., Kurup, D. B., De Taboada, L., Carroll, J. D., & Hamblin, M. R. (2010). Effect of pulsing in low-level light therapy. Lasers in surgery and medicine, 42(6), 450–466. https://doi.org/10.1002/lsm.20950.
