Highlights
- A small negative pressure dressing on the thigh boosted local blood flow by up to ~150% and increased tissue oxygen by around 25–28%.
- Circulation also improved in the opposite, untreated leg, showing a clear “remote” effect.
- A cyclic pattern (alternating stronger and milder suction) tended to produce the largest local and remote microcirculatory changes.
- Surface pressure under the dressing increased to about 30 mmHg, supporting better venous drainage and arterial inflow.
- This preclinical study suggests that a local negative pressure stimulus can enhance microcirculation both under the dressing and in a remote, untreated limb, supporting the concept of remote conditioning effects that may be relevant for future therapeutic strategies.
Why Microcirculation and Negative Pressure Matter
Our tissues depend on a dense network of tiny blood vessels — the microcirculation — to deliver oxygen and nutrients and remove waste. When microcirculation is sluggish, healing slows and tissues become more vulnerable.
Negative Pressure Wound Therapy (NPWT) uses a foam or dressing connected to a small pump to gently pull tissue upward with suction. It’s widely used in hospitals to help difficult wounds heal, but its direct effects on microcirculation — especially away from the treated area — are still being explored.
A 2022 human study in Frontiers in Surgery took a closer look at exactly this question:
Can a local negative pressure stimulus improve microcirculation both under the dressing and in distant tissue?
How the Study Worked
Researchers in Germany recruited 45 healthy young adults. A small NPWT foam dressing was placed on one thigh, and microcirculation was measured using a device that combines laser-Doppler and white-light spectroscopy.
They tracked four key parameters:
- Blood flow (BF)
- Tissue oxygen saturation (StO₂)
- Relative hemoglobin content (rHb)
- Red blood cell velocity (VELO)
Participants were randomized to one of three 60-minute suction patterns:
- Continuous: −120 mmHg for 60 minutes
- Intermittent: cycles of −120 / 0 mmHg (10 min each)
- Cyclic: cycles of −120 / −60 mmHg (10 min each)
Microcirculation was measured for 10 minutes before suction, 60 minutes during suction, and 30 minutes after suction stopped.
Local Effects: Strong Boost in Blood Flow and Oxygen
Under the dressing, all three negative pressure patterns significantly improved microcirculation:
- Blood flow roughly doubled or more in many time points, with maximum increases up to about +150% vs. baseline in the cyclic group.
- Tissue oxygen saturation (StO₂) rose by about +25–28% compared with baseline.
- Relative hemoglobin content and red blood cell velocity also increased over time.
Interestingly, peak values often occurred after suction was turned off, suggesting a strong, lasting response in the tiny vessels.
Although the cyclic mode tended to produce the highest peak values for blood flow and velocity, statistically there were no major differences between modes in this healthy group.
Remote Effects: Circulation Changes in the Opposite Leg
The most intriguing finding came from the untreated thigh.
Even on the side without a dressing, the researchers observed:
- A steady, almost linear increase in blood flow over 60–90 minutes
- Increases in tissue oxygen saturation
- Noticeable changes in hemoglobin content and red blood cell velocity
In other words, a local negative pressure stimulus on one limb was enough to trigger a measurable circulatory response in the other limb.
The cyclic mode again tended to show the strongest remote effects, particularly for blood flow and red blood cell velocity, reinforcing the idea that repeated changes in suction may act as a more powerful circulatory “signal.”
This fits with concepts like Remote Ischemic Conditioning, where a controlled stimulus in one limb can influence circulation and protection in distant tissues.
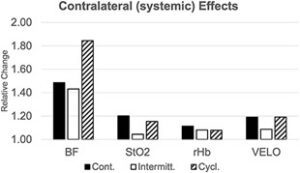
Figure 6. Remote (opposite-leg) circulation changes during negative pressure therapy. This graph shows how blood flow and related measures changed in the contralateral thigh (the leg without the dressing) 60 minutes after negative pressure was applied to the other leg. The value 1.0 on the y-axis represents each person’s baseline; bars above 1.0 mean an increase. BF = Blood flow; StO₂ = Tissue oxygen saturation; rHb = Relative hemoglobin contente; VELO = Red blood cell velocity. The different bar styles represent the three suction patterns: continuous (solid), intermittent (gray), and cyclic (striped). All modes increased circulation in the opposite leg, with the cyclic pattern showing the largest rise in blood flow and cell velocity.
How Might This Work?
Based on their data and prior work, the authors suggest a simple but powerful mechanism:
- Negative pressure increases surface pressure under the dressing (up to ~29 mmHg).
- This likely enhances venous drainage from the area.
- Better venous outflow allows more arterial blood to flow in, raising blood flow and oxygen supply.
- Repeated cycles of suction (as in cyclic mode) may act like a stimulus that the body “reads,” triggering broader vascular responses and remote microcirculatory changes.
It’s a reminder that the vascular system is highly interconnected — what happens in one region can influence circulation elsewhere.
Take-Home Message
A small negative pressure dressing on the skin doesn’t just act locally — it appears to send a circulatory signal that:
- Boosts blood flow and oxygenation under the dressing, and
- Influences microcirculation in distant tissues as well.
For clinicians, researchers, and device developers, this study helps explain how local negative pressure can have both local and remote circulatory effects, and why the pattern of suction (continuous vs. intermittent vs. cyclic) might matter when designing future therapies.
Reference: Sogorski A, Becker A, Dadras M, et al. Superior Enhancement of Cutaneous Microcirculation Due to “Cyclic” Application of a Negative Pressure Wound Therapy Device in Humans – Local and Remote Effects. Front Surg. 2022;9:822122. Published 2022 Mar 3. doi:10.3389/fsurg.2022.822122
