Highlights:
- Early oxygenation support: In the ARDS-mode group, blood oxygen (PaO₂) increased from 65 to 77.5 mmHg on day 1, suggesting improved oxygenation soon after starting sessions.
- Improved CO₂ clearance over 3 days: In the pneumonia-mode group, carbon dioxide (PaCO₂) decreased from 43.6 to 34.8 mmHg, pointing to better ventilation efficiency across the short protocol.
- Simple, time-efficient protocol: The intervention was just 5 minutes per day for 3 consecutive days, added alongside standard COVID-19 treatment.
- Non-invasive, frequency-specific approach: Two distinct frequency modes were used to support different respiratory patterns (20–300 Hz for ARDS mode; 120–300 Hz for pneumonia mode).
A recent clinical study explored whether vibroacoustic therapy — targeted sound vibrations applied to the chest — could support patients with COVID-19–related respiratory failure, including complications associated with acute respiratory distress syndrome (ARDS) and pneumonia.
Key Findings
Oxygenation Improvements (ARDS Group)
On the first day of therapy, patients receiving treatment in the ARDS mode showed a significant rise in blood oxygen levels (PaO₂). Average PaO₂ increased from 65 mmHg to 77.5 mmHg, suggesting improved oxygenation shortly after the intervention began.
Carbon Dioxide Elimination (Pneumonia Group)
For patients treated in the pneumonia mode, carbon dioxide levels (PaCO₂) decreased over three days. Average PaCO₂ dropped from 43.6 mmHg to 34.8 mmHg, indicating a potential improvement in carbon dioxide clearance and breathing efficiency.
Authors’ Interpretation
The researchers concluded that vibroacoustic stimulation may be beneficial in both ARDS and pneumonia contexts. Using sound vibrations tailored to specific frequency ranges, the approach may support respiratory mechanics and gas exchange. While the results are encouraging, the authors recommend larger studies to confirm clinical effectiveness.
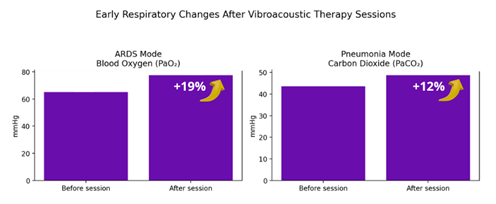
Figure 1. Early Respiratory Changes Observed After Vibroacoustic Therapy Sessions. Bar charts illustrate average respiratory gas measurements before and after a vibroacoustic therapy session in two treatment modes. Left panel: In the ARDS mode, mean arterial oxygen pressure (PaO₂) increased from 65 to 77.5 mmHg, corresponding to an approximate 19% increase, indicating improved oxygenation immediately after the session. Right panel: In the Pneumonia mode, mean arterial carbon dioxide pressure (PaCO₂) changed from 43.6 to 48.7 mmHg, corresponding to an approximate 12% change after the session.
Values represent group averages from a pilot clinical study; results reflect early physiological responses following short, frequency-specific vibroacoustic stimulation sessions.
How Vibroacoustic Therapy Works
Vibroacoustic therapy uses low-frequency sound waves to generate gentle vibrations that may help support breathing by promoting airflow dynamics and assisting with secretion mobilization. This type of non-invasive stimulation may be especially relevant in settings where respiratory function is compromised.
In the study, patients completed daily sessions (5 minutes each, for 3 consecutive days) in addition to standard COVID-19 treatment. Two operational modes were tested:
- ARDS Mode: 20–300 Hz, designed to target deeper lung tissues
- Pneumonia Mode: 120–300 Hz, designed to support upper airway drainage
Conclusion
This pilot study adds to growing interest in non-invasive supportive therapies for respiratory recovery. Frequency-specific vibroacoustic stimulation was associated with early improvements in oxygenation and carbon dioxide handling in patients with COVID-19–related respiratory failure. As larger trials are conducted, this approach may become an increasingly relevant option within respiratory support and rehabilitation strategies.
Reference: Konkayev A, Bekniyazova A. Vibroacoustic therapy in the treatment of patients with COVID-19 complicated by respiratory failure: a pilot randomized controlled trial. Front Med (Lausanne). 2023;10:1225384. Published 2023 Dec 14. doi:10.3389/fmed.2023.1225384
Link to full paper: Read here
